Table of Contents
Preface
Introduction
The Sonny Burke Story
Chapter I What is Thoracic Outlet Syndrome? (TOS)
Chapter II Anatomy
Chapter III The TOS Controversy
Chapter IV History, Cause, and Patient Presentations
Chapter V Physical Examination Findings
Chapter VI Diagnostic Tests
Chapter VII Standard of Care Approaches – Surgical and Non-Surgical
Chapter VIII Frequently Asked Questions
Chapter IX Case Histories of Patients
Chapter X The Human Spring Approach to Treatment and Prevention
Chapter V
Physical Examination Findings
Cervical Range of Motion
Cervical range of motion and flexion. We have a decreased range of motion and stiffness in the lower cervical and upper thoracic area. Cervical range of motion that I have seen is not the most prevalent range of motion but it is apparent and the patients usually complain of pain in the upper thoracic area around C6, C7, and T1. Extension when they extend the back, they feel a pinching sensation in the first and second thoracic ribs in the spine area. Their rotation usually is pretty good. I find that most of them can rotate about 70 – 75 degrees.
Rotation is not as significantly altered as lateral flexion. With these patients you try lateral flexion, and they’re getting maybe 5, 10 or at the most 15 degrees when normal is 45 degrees. Also what you’re seeing in lateral flexion is that when you laterally flex the left, the right scalene will become prominent. You place your finger on it and it feels so tense. It feels like a palpable hard band and it’s very stiff. When the range of motion in the cervical area and the anatomical structures are affected as well as the biomechanics become abnormal in the neck area.
Spasms in the Scalenes
In this particular slide, we’re talking about postural evaluation. What you’re going to do is sit in a chair in your office and you’re going to demonstrate the posture that the patient is in that causes the tension on the anterior scalene muscles which is the gentleman in the bottom picture and the lady who is leaning back in the chair. You and I both know that this is how many of us and a lot of children sit; and a lot of people have thoracic outlet syndrome.
Swelling in the supraclavicular area and around the neck
The swelling in a supraclavicular space is amazing to me because it’s so obvious and so blatant but few doctors ever notice it. I have had numerous patients who have come to me with swelling in the supraclavicular space. They have been to several physicians, none of which has made comments in their notes. The swelling comes from the inflammation, which results from the joint inflammation.
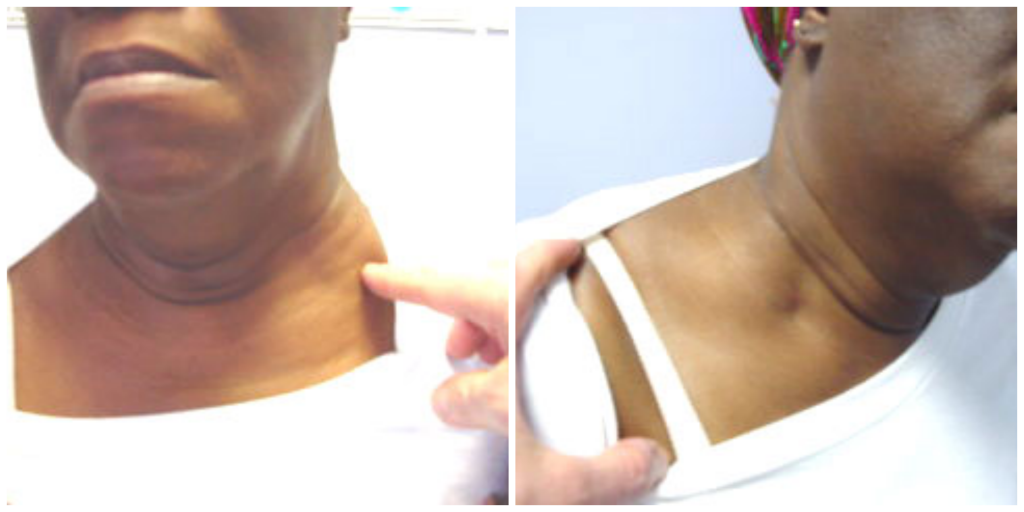
Example of Sever Supraclavicular swelling
As you can see on the top picture here, you can see the upper border of the clavicle on the patient and this patient below was involved in a motor vehicle accident at a fairly high speed. She has bilateral thoracic outlet syndrome. As you can see from the photograph, the superior border of the clavicle is obliterated. Also, you don’t see the sternocleidomastoid muscles and we don’t see any muscles structure in these patients and they are thin. In thinner patients, it is more obvious. There is really no fat there. So it’s not fat, it’s swelling. You should look for swelling of the supraclavicular space in your patients.
TOS can be subclinical and still signs of supraclavicular swelling can be noted I have patients who come in my office for a lower back adjustment. They look at me and when I see the left side of the supraclavicular space is swollen,
I ask them “Do you have numbness in your left hand periodically, more than in your right hand?” In nine times out of ten, they’ll say, “Yes, and how did you know?” Like I’m a magician.
How did you know I had numbness in my hand?
There is no documentation in the forms the patient filled out where they note their symptoms? Nobody had mentioned to the staff or me about this symptom, and they weren’t even interested in discussing it with us. They came in for their lower back. It was an incident that had started approximately one, two or perhaps six months ago. But just by my observation, the supraclavicular space was swollen and the patient, I feel, had this thoracic outlet syndrome.
note; the example above shows how subtle the right hand swelling or edema can be. This patient did not realize the right hand was more swollen then the left. They started to see a difference when a photo was taken of both hands to compare the two.
Swelling in the hands
Usually it’s better to take a photograph of the hands and evaluate it that way. I found that this can be a very helpful tool, because sometimes you don’t see it at first, and it can be seen well through a photograph. The second thing is to look at the tendons. If the tendons have been obliterated by edema, you might be looking at a patient who has had difficulty in drainage of the blood from the extremity. It kind of balloons out and they’re going to get a little tingling – that’s when it’s starts to affect the arterial supply. In this situation, the patient becomes a little worried and it is at that time that the patient usually comes to see you.
These are actual pictures of patients that have thoracic outlet in my office. This particular patient that you see with the hands on the top picture is the lady in the previous picture that had the supraclavicular swelling. As you can see on the right hand, it is much larger than the left. In fact, this enlargement is a swelling and is a result of the fact that the venous return is blocked because of the superior rib subluxation or some intrascalene type of compression on the subclavian vein not allowing the blood to escape from the hand. On the lower picture, we have a gentleman who has the same syndrome.
Not only does his right hand appear to be bigger, but the wrist and forearm also appear to be bigger. I saw vaguely that there were some differences in the hands, but when I took a photograph of the patient, it became very obvious. My feeling is that this is something you should you use as a tool because it brings out the differences more strikingly.
Manual Muscle Testing and TOS Rotator Cuff Muscle Testing
Shoulder Orthopedic Tests Because of all the attachments in the neck and the shoulder area, you’re also going to find that the shoulder range of motion is going to be affected. It’s affected or decreased in 44% of thoracic outlet syndrome according to a very large study that I reviewed. What happens is the elevation of the first rib causes an ultra biomechanics of the shoulder, because se the shoulder articulates on the dome that is re presented by the first, second and third ribs. Therefore, if you’re going to alter the foundation by which the structure by which the structure moves upon, you’re going to cause damage to that structure. It’s no different from the structures of a building affecting the first, second and third floors. It’s very simple.
Rotator Cuff Syndrome and TOS
Other muscles originating from the chest, neck and shoulder are further affected predisposing the patient to rotator cuff syndromes and impingement syndromes. The first muscle that is affected is the superspinatus. I am going to demonstrate to you the biomechanics of what goes wrong. The first rib subluxates, causing a rising of the clavicle, and as a result added tension is placed on the superspinatus.
The superspinatus muscle test is usually weak, and I’d say that on 50 – 60% of those patients that have long standing thoracic outlet syndrome for more than 3 or 4 months. You need to also do an evaluation of the shoulder mechanism because this usually is the second area of emphasizing of the thoracic outlet syndrome.
Muscle groups that are commonly affected are the anterior cervical muscles as I mentioned to you because of the fact that you’re holding the muscles in a contracted position for a long time. These muscles should not be put in a contracted position for this long of a time and that’s why they become weak and spastic and lead to elevation of the first rib.
The supraspinatus as I had mentioned and also the latissimus dorsi intrinsic muscles of the fingers – when you’re doing your physical examination you should measure the strengths of the intrinsic muscles of the fingers because that’s the first area of weakness that you’re going to find that the patient will experience when they start to lose grip strength and strength in the hand as a result of a fairly lengthy compressive forces, the forces that are occurring in the brachial plexus, subclavian vein.
Rotator Cuff Muscle Testing
The rotator cuff in advanced cases does not take long to evaluate, and is necessary and important, therefore you should do it. In the x-ray findings, you’re going to find a loss or a cervical curve or a retrolisthesis, called a military spine, whiplash spine.
I don’t care what you call it. The bottom line is that either
- It’s straight or
- It’s curved in the opposite direction of the way it’s supposed to be.
What you have to understand is that the cervical curve is designed in such a way to function as a curve. If you take the spine out of its position and normal alignment, you’ll find that the joints are going to wear out faster. It’s compared to your vehicle being out of alignment; the tires are going to wear out faster. Any moving part of machinery, will wear out faster.
Tests and Diagnosis
Diagnosing thoracic outlet syndrome can be difficult because the symptoms and their severity can vary greatly among people with the disorder. To diagnose thoracic outlet syndrome, your doctor may do a physical exam and ask about your medical history.
Physical exam- Your doctor will perform a physical examination to look for external signs of thoracic outlet syndrome, such as a depression in your shoulder, a pale discoloration in your arm or limited range of motion.
Medical history- Your doctor will also likely ask about your medical history and symptoms, as well as your occupation and physical activities.
Provocation tests- Provocation tests are designed to reproduce your symptoms. The tests may help your doctor determine the cause of your condition, and also will help rule out other causes that may have similar symptoms.
Some of the more common provocation tests that can suggest the presence of thoracic outlet syndrome include:
(+) Hyperabduction Maneuver – Wrights Test
The Hyperabduction Maneuver or Wrights Test examines neural tissue compromise through thorac-coraco-pectoral gate or axillary interval. The patient is seated with arms at the side. The radial pulse is palpated. From a sitting position and with the help of your doctor, you’ll hold your arm up and back (hyperabduction), rotating it outward, while your doctor checks your pulse to see if it’s diminished. As in the Adson’s maneuver, your doctor will want to know if your symptoms are reproduced during the test.
This will place a strain on the thoracic outlet bundle and subclavian artery vein and, the brachial plexus because if the pectoralis is in a spasm or tension, not allowing the shoulder to move properly, then of course, the nerve and vascular structures will be compromised and the patient will have symptoms. What you’re talking about is abduction at about 280 degrees, you’re going to take the radial pulse and it will elicit a decrease or diminish radial pulse or you will not be able to feel the radial pulse at all.
(+) Roos Test
The patient complains of subsequent numbness immediately following the test. Now normally nerves don’t act that way; usually vascular structures act that way. The elevated arms test or Roos test is considered the most reliable test for thoracic outlet syndrome where the patient is placed in this position, opening and closing the hand for approximately 3 minutes. You know, the movement of the hand should stimulate blood flow into the arm, but in these particular patients, blood flow is not good enough due to the compressive forces that are brought out by the malposition of the ribs and the structures in the thoracic outlet area. So this is the most reliable.
(+) Adsons Test
The Adson’s maneuver is when a patient takes a deep breath and holds it. As the patient takes a deep breath, obviously, the thoracic ribs will elevate. Holding the breath will keep the ribs in that position. They are going to hyperextend the neck, which is going to cause the scalene muscles to be stretched back across the subclavian artery vein and the brachial plexus area. If the patient has an elevated rib, this involves the scalene muscles, in fact that will cut off the air supply or cause the compression of brachial plexus muscles and illicit the numbness. In fact, what we find is that the symptom is reduced arterial blood flow. There is no more pulse within 3 to 5 seconds. The patient then complains of numbness. You ask the patient, “Is your arm going numb?”. The patient answers “Yes, it is.”. You don’t say anything; the patient says “you know, I’m feeling some tingling sensations in my fingers. The costaclavicular test narrows the costaclavicular space by bringing the clavicle close to the first and second rib.
When the patient draws the shoulder downward, that causes the compression of the subclavian artery vein and the brachial plexus. Positive tests are when the radial pulse is diminished. These diagnostic tests are very good to show that there is some compressive force in the thoracic outlet area, but by no means do they point toward immediate surgery.
(+) Costoclavicular Test
False Positives suggest TOS is over diagnosed
Because I feel that this posture of leaning back to watch television, leaning back in the car in multiple positions, and many automobile traumas: everyone in the United States has had on average of at least one car accident in their life. Therefore, these traumas as well as sports injuries, to affect the anterior cervical area are so prevalent that I believe that some are clinical, and others subclinical. Some of these provocative tests were performed on normal individuals. These patients were probably not normal. More detailed evaluations of the motion of the first rib, certainly whether that rib was in a good position, or aligned properly or whether it was affected should have been performed. These evaluations were not done according to the literature. So we cannot say that false positives were elicited. But we may say that it’s a possibility that we found subclinical of thoracic outlet syndrome and not necessarily false positives. I hope you understand that.
Manual Muscle Testing
When evaluating thoracic outlet syndrome, one of the physical evaluations, which is very important in your physical, is you want to do manual muscle testing. A doctor who is astute in manual muscle testing can usually isolate muscles that have been put into a tonic protective spasm or a weakened position. After a lot of practice, you can become very skillful at this technique.
Superior Rib Subluxation or First Rib Motion Palpation
The spinal examination will yield a superior subluxation on one or both of the first ribs. Various different studies of motion of the first ribs having the doctor placing the thumb on the first rib in the back on the neck and actually tilting the head to the side in extension – what you’re finding is that rib does not move. Usually what is supposed to happen is that it is supposed to disappear down into the thorax and then bringing you back to allow it to reappear.
What you’re finding is that you have an endplate or end field, which is very stiff. Normal mobility does not disappear. It feels like it’s immobile; that’s when it’s not moving. What happened if the ribs do not move? Ribs have to move in order for normal respiration to occur. They have to move up and back. If the ribs do not move, the patient will have labored breathing.
The first rib can subluxate either from trauma or static postural stress from a car accident or sports injury. I feel that while trauma is a very significant source of damage to the neck, static postural stress is a more common cause of thoracic outlet syndrome. We are going to talk about that more. Some mention of static postural stress is made in the literature but it is my opinion that there needs to be more discussion of static postural stress as the cause of thoracic outlet syndrome.
Costal Chondral Junction Subluxation
Costal Chondral Junction Subluxations As we mentioned before, subluxation of the upper thoracic vertebral segments in costa chondral and costa junctions or joints- As I mentioned before, when the rib subluxates superiorly, due to the fact that it is connected through the intercostals muscles, to the 2nd, 3rd and 4th ribs. What you’ll find here is arthritic changes. I’m going to go over that in a minute. You’re going to look for that on the radiographs you’re going to look at the chondral costal junctions, costal vertebral transverse junctions, and you’re going to look for increase in the white calcium deposits and buildup of white calcium deposits on these joints.

“I believe that locating the exact area of nerve compression is important, but what I have been finding in my clinical work is that the majority of these tests are positive when you have thoracic outlet syndrome. Doctors complain these tests create many false positives. There very well could be a valid explanation for this. When the first rib elevates and causes a compressive force upon the brachial plexus, subclavian vein and artery, then we would say that the rib, is subluxated to a large degree.”
–Dr. James Stoxen DC
READ MORE POSTS ON THORACIC OUTLET SYNDROM
www.thoracicoutletsyndrome.com