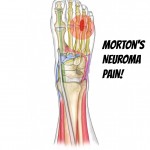
Morton’s Metatarsalgia ICD-9 355.6 Morton’s Neuroma - Self Help Tips, Treatment and Prevention From The Barefoot Running Doctor at Team Doctors Tips For Better Health Ask the doctor, Dr. James Stoxen DC In this article is everything you ever wanted to know about Morton’s neuroma and more! Is your foot hurting? Do you have tingling in the feet or burning feet? Do you have foot aches and do you have toe numbness? The “Morton’s Metatarsalgia ICD-9 355.6” (pain between … [Read more...]
Dr. James Stoxen DC Has Been Appointed to the Advisory Board for the American Board of Anti-Aging Health Practitioners and The American Board of Anti-Aging /Regenerative Medicine
Dr. James Stoxen DC Has Been appointed to the Advisory Board for the American Board of Anti-Aging Health Practitioners (ABAAHP) and The American Board of Anti-Aging /Regenerative Medicine (ABAARM) The American Board of Anti-Aging Health Practitioners was founded in 1999 to provide advanced education, representation, and specialty recognition of scientific and healthcare professionals. The long-term objective of ABAAHP is to achieve formal sub-specialty recognition and a new … [Read more...]
Doc Gringeri and Dr. Stoxen Visit The Wiggles Show!
Doc Gringeri and Dr. Stoxen Visit the Wiggles Show! … [Read more...]
Video Tutorial #202 When my feet hurt.. I did this pressure point and got relief.
MY FEET HURT! Tips For Better Health Ask the doctor, Dr James Stoxen DC I remember standing on my feet all day 14 - 16 hours a day for 135 days in a row on one of those runs when I was getting calls from so many big name entertainers that I could not say, NO! But I ended up with sore toes, pain on the bottom of the foot pain on the side of the foot. Lets just say my feet were in pain! I also remember I had pain in the big toe like a turf toe. I did this deep tissue treatment for … [Read more...]
Video Testimonial – Dr. James Stoxen DC – National College of Chiropractic Grad 1986
This is a video testimonial I am proud to have done about National University Health Sciences, formerly National College of Chiropractic. My father Dr Paul Stoxen DC graduated there in 1949 and I graduated there in 1986. They really did a great job in preparing me for my career as a chiropractor. I highly recommend NCC! Meet Dr. James Stoxen DC, who graduated from National in 1986: I choose National because it offered the chiropractic component and more … [Read more...]
RADIO INTERVIEW: Dr. James Stoxen DC Live On FOX Newsradio 910 WSBA – Tuesday 6:10 am, May 15, 2012 Listen to it live anywhere!
Dr. James Stoxen DC will be live on FOX NewsRadio 910 WSBA The York's Morning News at 6:10am East York, PA With with MARK McKENZIE, JIM HORN and GARY SUTTON Listen to the interview live from anywhere by clicking here … [Read more...]
USA TODAY – Wiggles Founder, Anthony Field and Dr. James Stoxen DC Appear In The Champions of Chiropractic, Advertorial In USA Today
Hi Friends, This is the article that appeared in the USA Today Newspaper on Thursday, April 26th, 2012 while I was lecturing in Malaysia. I finally got a copy. The Champions of Chiropractic is an appropriate title for Anthony Field, a champion for children, treated by Team Doctors, Treatment and Training Center of Champions. Working with Anthony Field has been a very rewarding victory! Huge thanks to the Foundation For Chiropractic Progress for … [Read more...]
Media Alert!!! CNN, Anthony Field and Dr. James Stoxen Interview With Shannon Cook Airs Saturday, August 4th
Be sure to tune in Saturday, August 4th as Dr. James Stoxen DC is Interviewed by Shannon Cook about his treatment approach that helped Anthony Field back to health. Dr. Stoxen's treatment approach, 'The Human Spring Theory', which states: The human spring stores mechanical energy therefore it is an efficiency mechanism. The human spring provides the protective mechanism for the body. The human spring allows us to land our bodies on uneven surfaces by adjusting the body … [Read more...]
FRONT PAGE ARTICLE – Tuned To the Power of Chiropractic Care – The Story of How Anthony Field Got His Wiggle Back
Wiggling To Wellness With Chiropractic Care written by Brenda Duran, Senior Associate Editor Dynamic Chiropractic – April 22, 2012, Vol. 30, Issue 09 Great News!!! Don Peterson put a fantastic article on the front page of the Dynamic Chiropractic Magazine this week! Dynamic Chiropractic is the most widely read magazine in the chiropractic profession with over 40,000 readers worldwide. This is a huge surprise and will bring a huge amount of interest and … [Read more...]
Wiggles Media Blitz! Today Show! ABC! CBS! NBC! FOX! CNN! MSN!
Depression ICD-9 296.3, Chronic Fatigue Syndrome ICD-9 780.71, Fibromyalgia ICD-9 729.1 Champions Of Chiropractic: Wiggles Media Blitz! Taken from the excerpt from the Foundation for Chiropractic Progress newsletter Anthony Field praises chiropractic on the Today Show, ABC, CBS, NBC, FOX, CNN and MSN! Greetings, The Foundation for Chiropractic Progress (F4CP) is excited to announce that it,s spokesperson, Anthony Field, creator and member of the popular … [Read more...]
The Foundation For Chiropractic Progress Officially Announces Anthony Field (Wiggles) As A Spokesperson For 2012 At The Parker Seminar Las Vegas
The Foundation for Chiropractic Progress, Officially announces Anthony Field (Wiggles) as a Spokesperson for 2012 at the Parker Seminar Las Vegas. The event started off with a very classy fashion show produced by Dillards Department Stores featuring Foundation board members modeling Dillards clothing. All purchases of Dillards clothing that weekend yielded a 10% donation to the foundation. Board members modeling in this show featured Carol Ann Malizia, DC, Dr. Fabrizio Mancini, … [Read more...]
Wiggling His Way to Wellness, To Your Health Magazine, December, 2011
Wiggling His Way to Wellness To Your Health Magazine By Brenda Duran December, 2011 (Vol. 05, Issue 12) To read the article go to: http://www.toyourhealth.com/mpacms/tyh/article.php?id=1473 Anthony Field is one of the founding members of "The Wiggles," whose popular children's television show has spawned CDs, DVDs and even live concerts. Entertaining and teaching children is Field's passion, but the rigors of the job were taking a toll on his health. That's why Field … [Read more...]
Insights Into Anti-aging Chiropractic: 7 DCs Talk About Their Anti-aging Practices
7 DCs Talk About Their Anti-aging Practices By John V. Wood Original Article: http://www.chiroeco.com/news/print-this.php?id=1843 The American Academy of Anti-Aging Medicine (A4M, www.worldhealth.net) claims that 100 million Americans are currently being treated for one or more degenerative diseases at a healthcare cost of more than $700 billion per year. A4M believes if medical professionals really want to make an impact on healthcare in this country and the world, they must focus … [Read more...]